Overview
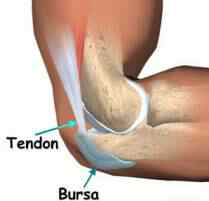
Pain of the Achilles tendon commonly affects both competitive and recreational athletes, and the sedentary. The largest tendon in the body, the Achilles tendon, endures strain and risks rupture from running, jumping, and sudden acceleration or deceleration. Overuse, vascular diseases, neuropathy, and rheumatologic diseases may cause tendon degeneration. The hallmarks of Achilles tendon problems seem to be damaged, weak, inelastic tissue. Causes A rupture occurs when a patient overstretches the Achilles tendon, an act which causes it to tear partially or completely. Achilles tendon ruptures can occur during athletic play or any time the tendon is stretched in an unexpected way. Symptoms You may notice the symptoms come on suddenly during a sporting activity or injury. You might hear a snap or feel a sudden sharp pain when the tendon is torn. The sharp pain usually settles quickly, although there may be some aching at the back of the lower leg. After the injury, the usual symptoms are a flat-footed type of walk. You can walk and bear weight, but cannot push off the ground properly on the side where the tendon is ruptured. Inability to stand on tiptoe. If the tendon is completely torn, you may feel a gap just above the back of the heel. However, if there is bruising then the swelling may disguise the gap. If you suspect an Achilles tendon rupture, it is best to see a doctor urgently, because the tendon heals better if treated sooner rather than later. A person with a ruptured Achilles tendon may experience one or more of the following. Sudden pain (which feels like a kick or a stab) in the back of the ankle or calf, often subsiding into a dull ache. A popping or snapping sensation. Swelling on the back of the leg between the heel and the calf. Difficulty walking (especially upstairs or uphill) and difficulty rising up on the toes. Diagnosis A typical history as detailed above together with positive clinical examination usually will clinch the diagnosis. In an acute rupture, one can usually feel the gap in the tendon from the rupture. There may be swelling or bruising around the ankle and foot of the injured leg. With the patient lying on the tummy (prone position) with the knee flexed, the examiner should see the ankle and foot flex downwards (plantarward) when squeezing the calf muscles. If there is no movement in the ankle and foot on squeezing the calf muscle, this implies that the calf muscle is no longer attached to the heel bone due to a complete Achilles tendon rupture. Non Surgical Treatment Your doctor may advise you to rest your leg and keep the tendon immobile in a plaster cast while it heals. Or you may need to have an operation to treat an Achilles tendon rupture. The treatment you have will depend on your individual circumstances, such as your age, general health and how active you are. It will also depend on whether you have partially or completely torn your tendon. If you have a partial tear, it might get better without any treatment. Ask your doctor for advice on the best treatment for you. If you need pain relief, you can take over-the-counter painkillers such as paracetamol or ibuprofen. Always read the patient information that comes with your medicine and if you have any questions, ask your pharmacist for advice. 
Surgical Treatment Regaining Achilles tendon function after an injury is critical for walking. The goal of Achilles tendon repair is to reconnect the calf muscles with the heel bone to restore push-off strength. Those best suited for surgical repair of an acute or chronic Achilles tendon rupture include healthy, active people who want to return to activities such as jogging, running, biking, etc. Even those who are less active may be candidates for surgical repair. Non-operative treatment may also be an option. The decision to operate should be discussed with your orthopaedic foot and ankle surgeon. Chiropractics is a simple human manual therapy used to diagnose medical conditions in humans and animals. For a long time, doctors and non-doctors alike have been recommending the painkiller acetaminophen (paracetamol) — more popularly known as Tylenol — for a wide array of pains, including lower back pain.  As sufferers of back pain can attest, often times, surgery to correct these problems doesn't work. Either the back pain remains after the surgical procedure or it is exacerbated by the surgery, causing patients to undergo further surgeries or become dependent on medications to seek relief. Dr. Randy Laurich helps patients break the cycle of pain, medication, and surgery by treating back pain with cutting edge chiropractic methods, such as the DRX9000, and other holistic methods. At the Wellness Experience, Dr. Randy Laurich works with a team of doctors and medical professionals to address all aspects of back pain. The professionals at The Wellness Experience are able to incorporate into your pain treatment acupuncture, exercise, massage, and laser therapy where appropriate so that all sources of pain are being addressed. The SpineMED Table is specifically designed to treat these types of conditions. One Month later, my pain had decreased by 50 %. It is now just over two months into the program, and I can honestly, and amazingly, say that I am 98% pain free. People who have suffered with back pain for years will find relief with your program. I should know because I've seen these exercises work wonders for young and not-so-young. For the past 12 years, I have hardly had a pain free moment with my the past 8 years I have gone to the Chiropractor every week and sometimes two and three times, and I was told there my pelvic area shifts out of place. I woke up this morning with severe pain and was feeling a bit panic'd. As sufferers of back pain can attest, often times, surgery to correct these problems doesn't work. Either the back pain remains after the surgical procedure or it is exacerbated by the surgery, causing patients to undergo further surgeries or become dependent on medications to seek relief. Dr. Randy Laurich helps patients break the cycle of pain, medication, and surgery by treating back pain with cutting edge chiropractic methods, such as the DRX9000, and other holistic methods. At the Wellness Experience, Dr. Randy Laurich works with a team of doctors and medical professionals to address all aspects of back pain. The professionals at The Wellness Experience are able to incorporate into your pain treatment acupuncture, exercise, massage, and laser therapy where appropriate so that all sources of pain are being addressed. The SpineMED Table is specifically designed to treat these types of conditions. One Month later, my pain had decreased by 50 %. It is now just over two months into the program, and I can honestly, and amazingly, say that I am 98% pain free. People who have suffered with back pain for years will find relief with your program. I should know because I've seen these exercises work wonders for young and not-so-young. For the past 12 years, I have hardly had a pain free moment with my the past 8 years I have gone to the Chiropractor every week and sometimes two and three times, and I was told there my pelvic area shifts out of place. I woke up this morning with severe pain and was feeling a bit panic'd. Also, there are special soles which can be used in shoes and sandals to help reduce the back pain. These soles have specific pressure points that ease the pain while walking. What's more, hormonal changes in pregnancy loosen your joints and the ligaments that attach your pelvic bones to your spine. This can make you feel less stable and cause pain when you walk, stand, sit for long periods, roll over in bed, get out of a low chair or the tub, bend, or lift things. As many as three-quarters of pregnant women experience back pain at some point. Most often the pain appears in the later months or becomes worse as pregnancy progresses. It may also persist after the baby arrives, but postpartum back pain usually resolves in a few months. Some women have symptoms of both types of low back pain. Lumbar pain is like the low back pain you may have experienced before you were pregnant. More the number of hours spent exercising, more will be the reduction in the risk of chronic pain. Obese men and women are more likely to suffer from chronic back and neck pain. When he launched the concept in 1981, he explained that extending the spine can help relieve back pain in most patients. The three steps involved in treating a patient with lower back pain caused due to some problem related to spine and extremities are assessment, treatment, and prevention. This is the point where I really get to doubt evidence and start believing more in experience… I'm perfectly well acknowledging that people with soft, functional muscles and normal joint play can have whatever posture they want without great implication on pain. Best example is the psoas: I know that it supposedly cannot shorten from sitting and so on, but in real life, treating the psoas is my number one solution for people with hyperlordosis and lower back pain. Up to 80% of any given population experience and suffer from either acute or chronic forms of this pain. It can begin as early from school age and well into the senior years with 35-55 years of age being the most affected. Fewer than 5% of people who suffer from back pain are suitable candidates for surgical treatment. The lower or upper left back pain is due to an injured muscle. Upper back pain causes can vary significantly which is why understanding the various and symptoms and components of upper back pain can help to determine how the back was injured. This understanding will also result in valuable insight when considering treatment options. Treatment usually includes spinal manipulation by a chiropractor, physiotherapy and anti-inflammatory medication. Spasms are characterized by spontaneous, abnormal contractions of the muscles in the upper back. One of the causes of upper back pain is poor neck posture which ultimately pushes the area between the shoulder blades out as the head goes forward. This is probably the least common cause of upper back pain. Also, there are special soles which can be used in shoes and sandals to help reduce the back pain. These soles have specific pressure points that ease the pain while walking. What's more, hormonal changes in pregnancy loosen your joints and the ligaments that attach your pelvic bones to your spine. This can make you feel less stable and cause pain when you walk, stand, sit for long periods, roll over in bed, get out of a low chair or the tub, bend, or lift things. As many as three-quarters of pregnant women experience back pain at some point. Most often the pain appears in the later months or becomes worse as pregnancy progresses. It may also persist after the baby arrives, but postpartum back pain usually resolves in a few months. Some women have symptoms of both types of low back pain. Lumbar pain is like the low back pain you may have experienced before you were pregnant. More the number of hours spent exercising, more will be the reduction in the risk of chronic pain. Obese men and women are more likely to suffer from chronic back and neck pain. When he launched the concept in 1981, he explained that extending the spine can help relieve back pain in most patients. The three steps involved in treating a patient with lower back pain caused due to some problem related to spine and extremities are assessment, treatment, and prevention. This is the point where I really get to doubt evidence and start believing more in experience… I'm perfectly well acknowledging that people with soft, functional muscles and normal joint play can have whatever posture they want without great implication on pain. Best example is the psoas: I know that it supposedly cannot shorten from sitting and so on, but in real life, treating the psoas is my number one solution for people with hyperlordosis and lower back pain. Up to 80% of any given population experience and suffer from either acute or chronic forms of this pain. It can begin as early from school age and well into the senior years with 35-55 years of age being the most affected. Fewer than 5% of people who suffer from back pain are suitable candidates for surgical treatment. The lower or upper left back pain is due to an injured muscle. Upper back pain causes can vary significantly which is why understanding the various and symptoms and components of upper back pain can help to determine how the back was injured. This understanding will also result in valuable insight when considering treatment options. Treatment usually includes spinal manipulation by a chiropractor, physiotherapy and anti-inflammatory medication. Spasms are characterized by spontaneous, abnormal contractions of the muscles in the upper back. One of the causes of upper back pain is poor neck posture which ultimately pushes the area between the shoulder blades out as the head goes forward. This is probably the least common cause of upper back pain. |
 RSS Feed
RSS Feed